How Many C’s Are In Success?
Maureen Hazen, RN, MHA, Associate Director, Berkley Research Group’s Healthcare Practice and Robert Andrzejewski, MS, Associate, Berkley Research Group’s Healthcare
In today’s economic environment, hospitals are being forced to make some deep rooted cultural changes to succeed. Leaders take responsibility for the direction of their teams but are also tasked with creating vision, bringing tools, raising accountability, and improving the quality of a team’s output. One of the keys to overall success in completing all of the tasks listed is providing communication. The frequency, potency, and specificity of communication is essential. Hospital staff need to be aware of healthcare challenges but more specifically their hospital’s financial state of affairs. Cascading this information throughout an organization can be both empowering and transformational. When people are “in the know” they are more inclined to participate and feel a part of the team. Staff can be insightful regarding cost containment and should be encouraged to share their ideas and recommendations for cost containment. Providing transparency into specific department costs/operations will allow everyone to understand the big picture and provide motivation to look for ways to lower costs while continuing to provide high quality care to patients.
With strong leadership, staff involvement and successful teams, hospitals can work to achieve cost containment. Refocusing product review teams to look at consumption and utilization practices will identify many savings that have not traditionally been approached. The key is to monitor and report successes through dashboards.
Hospital Product Review Processes
Many hospitals have various avenues that can be used to present cost avoidance, cost reduction, as well as revenue generation ideas. Whatever the name of your hospital cost containment team/process, (Product Review, Value Analysis, Product Acquisition and Management, Utilization Management, Cost and Value, Cost Effectiveness, etc.), they are all vehicles to look at every aspect relevant for assessing the total cost of products, practices, and processes. These teams should not be perceived as a short-term answer but instead a methodology to achieve sustainable solutions.
Identifying All the C’s In a Successful Team
Although there are only two C’s in success, when it comes to building a successful team focused on cost containment there are actually several C’s to success. Identifying and applying the many C’s in success into your cost containment processes can assist to create a more dynamic team. When assessing the effectiveness of your team you may want to consider evaluating each of the following components.
- Commitment/Contribution
- Team members are committed to accomplishing a mission and expected outcomes.
- Team members contribute insight and out-of-the-box ideas.
- Competency
- Competent team members provide trust and credibility that they will deliver quality outcomes.
- Communication/Coaching
- Team members should always be free to speak within the team, ask questions, and seek clarification and to communicate constructively in a positive and respectful manner.
- Team members must be educated and coached by a committed project champion in order to understand the scope of the project and action items required to be successful.
- Cooperation/Collaboration
- Work together to achieve a common goal. Team members should be able to figure out ways to work together to solve problems and accomplish the end goal.
- Collaboration is working with others to complete a task and achieve shared goals.
- Culture/Celebration
- Team members share beliefs and goals.
- Recognize team members for hard work and contributions.
- Clean Data
- Clean and accurate data is a key factor when analyzing and making recommendations based off of numbers. Data must be checked for quality prior to analysis, otherwise you run the risk of “garbage in, garbage out.” Once data has been proven inaccurate you have lost your credibility with key stakeholders.
Balancing the C’s can assist you to build a highly effective team. Taking an idea from conception to implementation with the end result of success is a great team motivator. The key is to involve the staff and include utilization initiatives to assist in bringing savings to the hospital’s bottom line.
What type of ideas should your teams be looking for?
Approaching Consumption/Utilization Practices
Driving down prices on medical supplies has historically provided good savings but often, vendors offer their own strategies for providing cost savings. An example is rebates which can often go unnoticed at hitting a department’s bottom line. A bigger and bolder step, which many hospital cost containment teams have not jumped into with both feet yet, is evaluating the appropriate consumption and utilization of products. Why is cost effective utilization so elusive? The thought provoking question to cost containment team members is: Do we have differences with consumption and utilization practices with products? Are products being used incorrectly or carelessly? Do we need to brainstorm with the team as to what products they perceive have different utilization practices and tour units and interview and shadow staff and physicians to understand the differences.
Look for the key to open ideas for utilization initiatives.
Below are some examples of different utilization practices that have been observed in hospitals. We need to determine which of these is a best practice.
- Usage of Large Disposable Underpads
- Placing multiple pads versus one on a patient bed
- Placing a large pad under an extremity for a blood draw instead of a smaller pad
- Lining bedside table draw
- Cleaning up spills
- Usage of Disposable Pulse Oximetry Probes
- Inappropriate sensors are placed on areas in an attempt to get a more accurate reading (i.e. forehead sensor placed on finger).
- All areas of the hospital do not have the same type of sensors, therefore, if a patient is transferred a new sensor may need to be placed.
- Blood Utilization
- Defining “appropriate” criteria for determining blood product transfusion action
- Ordering many blood products prior to a procedure
- Transfuse one unit RBC’s then reassess ongoing blood loss
Accurate Data and Dashboards
Accurate data rules when demonstrating the value of monitoring utilization practices. It provides actionable information. The challenge with many hospitals has been to identify then monitor utilization patterns. Presenting utilization data at the departmental/service line level provides the details that managers need to influence change. Trend lines need to be monitored. Most importantly, the analysis must quantify how the wasteful practices are financially impacting the hospital.
Software exists that the vendor states possesses the capability to identify and quantify products that are being over utilized. If purchasing software is not an option, models and tools for monitoring and tracking trends can be created using spreadsheet software such as excel. It will not identify the practice but can be used to trend the practice. For example:
When creating a dashboard that can be used to monitor and track savings for a utilization initiative, be aware of two things: What is the key performance indicator (KPI) to be used for calculating savings and what is the hospital benchmarking itself against? A KPI is a quantifiable measurement that can be used to track the savings and progress of an initiative.
Determine:
- The optimal KPI for a particular initiative
- What patient population is being impacted?
- All patients, inpatient, outpatient, specific type of patients, etc?
- What is the appropriate denominator that should be applied to calculate savings?
- Adjusted patient days, patient days, patient admissions, etc?
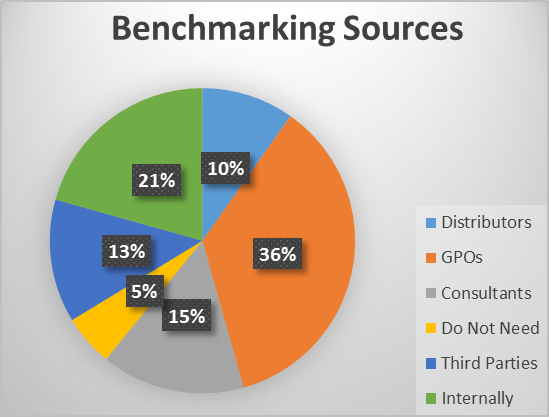
In regards to benchmarking, if a hospital does not own software that provides industry standards for utilization practices, then the best course of action is to benchmark against past performance and strive to improve upon that.
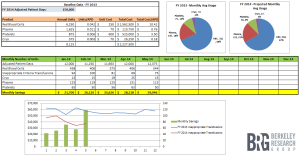
Below is an example of a dashboard used to track and monitor blood product utilization. Tools like this can clearly and effectively help a hospital be aware of how its product utilization is trending and validate savings.
Click charts to view full size
Conclusion
A results driven cost containment process should include the many C’s in success. Starting with a strong foundation of communication and incorporating the C’s into the team’s guiding principles is the key to building a sustainable process. Focusing your hospital’s cost containment process to having the team use the C’s in success, evaluating utilization practices, and monitoring/tracking initiatives will help you to achieve significant and sustainable long-term outcomes.
Maureen Hazen, RN, MHA
Maureen is an Associate Director at Berkeley Research Group’s Healthcare Practice. She has thirty years of clinical, managerial, education, and consulting experience. Maureen specializes in supply chain/product utilization and value analysis from identification through implementation of ideas. She provides thought leadership and subject matter expertise to support her client consulting engagements. Contact Maureen via email mhazen@thinkbrg.com
Robert Andrzejewski, MS
Robert is an Associate at Berkeley Research Group’s Healthcare Performance Improvement practice. Robert’s expertise includes analytics, performance improvement, and supply chain. His experience consists of implementing cost savings and revenue enhancing initiatives for academic medical centers and children’s hospitals. Contact Robert via email randrzejewski@thinkbrg.com